Patient Education
Biomechanical Orthotic Devices...
…may be made from various materials depending upon the degree of control required, the physical status, activities, occupation and footwear for each individual patient. Approximately 23 steps are required in their fabrication. They are made to conform to the desired contours of your feet and will vary in length and width if your feet also vary. The front edge of the orthotic device may appear to be short but always ends just BEHIND the weight bearing surfaces of the metatarsal heads and, therefore, does not take up additional room in the average shoe.
Most biomechanical orthotic devices appear narrower than the foot and when prepared for a woman’s shoe may appear to be as much as ½ to ¾ of an inch narrower on both sides. The biomechanical orthotic device should fit easily into the shoe without binding or spreading the heel or bulging out the sides. They are generally comfortable to wear after a short adjustment period and are usually worn initially in a build-up sequence during which time the patient gradually increases the daily wearing time.
In Addition...
… your Podiatrist/Chiropodist may prescribe a course of strapping, physio-therapy, manipulation or adjustment and may advise you to start one of the very popular and very beneficial flexibility or stretching programs consistent with your particular case and physical capabilities. Follow your practitioner’s instructions exactly. Do not be impatient and overdo things since this often diminishes the effectiveness of your therapy and actually tends to lengthen your response time. Remember, you cannot undo in a few weeks what it took years to create. Consult your practitioner immediately… hurting should not be part of your everyday life.
Would It Surprise You To Know...
…that a good part of your back trouble or hip pain or neck stiffness or knee clicking may be associated with or may be directly a result of poor foot function?
Probably it would.
Yet, you are undoubtedly aware of the annoying rock of a four-legged table when one leg is shorter than the rest. And what do you think would happen to your spine or hip or pelvis if you were to wear only one shoe with a one or two-inch platform added to it? And how many times have you seen the cracked walls in a new house whose foundation is ‘settling’ unevenly?
Well, identical things happen with the human body. While it is true that most people do not have one leg which is structurally shorter than another (that is, the bones are shorter), it is equally as true that vast numbers have what is known as a functional shortening of one leg. By this we mean that the foot which is composed of 26 main bones does have the ability to ‘flatten’ itself thereby dropping the ankle closer to the ground. In effect, the distance as measured from a point on the upper leg to the ground has shortened because of this flattening motion, and that is why it is called a functional shortening as opposed to a structural shortage.
To compensate for this action:
- The pelvis may tilt
- The spine my bend
- The opposite knee might bend
- You might move the longer leg out to the side putting stress on the hip or knee
- Or you might go through a combination of these compensating positions
Obviously, over a long period of time, things are going to change. Muscles may fatigue and spasm, bones may change their shapes and joints may be thrown out of line resulting in ‘wear and tear’
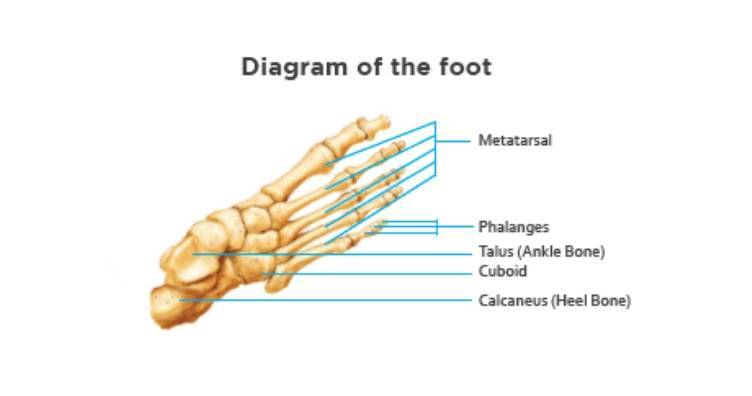
Something Else Can Also Happen
Suppose both feet flatten at the same time and to the same degree. Remember the 26 bones in the feet that we mentioned? Well the leg bone (the tibia), rests on the top bone in the foot called the talus. Not only is the talus one of the bones that makes up the ankle which is the joint at which you raise or drop your foot, but the talus is also capable of pivoting with a screw-like motion as it articulates with the heel bone just below it.
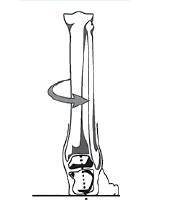
Try This
Make a fist with your right hand and then rotate your fist anti-clockwise as you move it forward, you will simulate the screw-like motion of the talus as the foot flattens. Also, notice that your entire arm rotates anti-clockwise as your leg does the same thing.
The Problem Occurs When...
What Do You Do About It?
Obviously, the pain is the ‘best’ symptom we have because it usually makes us go to the doctor. If you have obvious foot problems such as corns, calluses and bunions or foot aches, cramps, heel pain and fatigue, chances are four out of five that you are either a candidate for some postural problem or you already have one.
If you visit a Podiatrist, they will examine you to determine what your problem is and how it should be handled. They may contact your family doctor or specialist so that they can all work together to correct your condition and relieve your complaints.
If your practitioner is not a Podiatrist, they may suggest that you see one and arrange for a consultation or they may choose to handle your case themselves or in conjunction with a Podiatrist.
What Will Your Treatment Consist Of?
Today, there is a field in medical technology called Biomechanics; it is a fairly young, highly technical branch of medical engineering which deals in large part with human motion which helps us to determine limits of normality and abnormality.
As a result of this new work, biomechanically orientated practitioners have the ability to examine for biomechanical faults of the feet and legs, and therefore make certain determinations and diagnoses and establish a treatment plan.
As a major part of the treatment plan, biomechanical orthotic devices are custom made for the patient. These devices are commonly referred to as orthotics, but they have been referred to as foot appliances, inserts, plates and even arch supports. But even though they may look like old fashioned arch supports, the one thing they are NOT, is arch supports.
True biomechanical orthotic devices do not work on the principles of ‘supporting’ the arch. The impressions or casts which your practitioner will make of your feet will be taken in a specific position which will capture the angular relationships between the various segments of each foot.
Thus, when models of your feet are constructed at the laboratory, the evaluators and technicians will be able to ‘capture’ your best functioning positions in the models. Then, the bodies of the orthotic devices will be contoured and angled over these models.
Additional components called post controls will be added to the front, rear or both ends of the orthotic devices and will be ground to specific angles very much like spectacle lenses are.
Causes Of Your Pain
Treatment Available
Biomechanics Clinic Cardiff
To arrange an appointment at our Biomechanics clinic in Cardiff, please contact us. We can assess your condition then recommend an effective treatment solution based on your needs.